
What to Eat When Swallowing Fails?
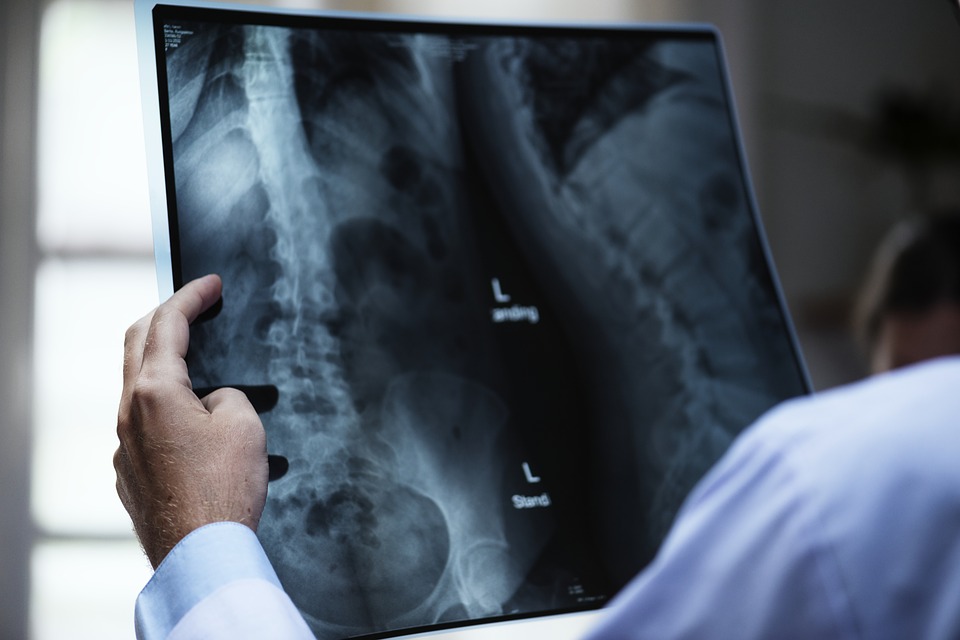
Swallowing. Most of us perform this apparently simple act many times every day without a second thought. Yet eating and swallowing is an extremely complex

Swallowing. Most of us perform this apparently simple act many times every day without a second thought. Yet eating and swallowing is an extremely complex
Nature, in her infinite intelligence, has gifted us millions of different proteins that supply the music and instruments of the body’s orchestra. These proteins are

Unless you are suffering a prolonged midlife crisis, life really does get better after 40—we can start to enjoy the fruits of our labour, care

When people think about causes of malnutrition, they might consider poor appetite, chewing difficulties or illness as likely candidates. Yet many health professionals would know

Just $6.08 per resident per day is the average spent on food and ingredients in Australian aged care facilities, according to a recent study. The

Obesity is one of the biggest health issues facing Australians today. It is forecast that 35% of Australians will be obese by 2025. What is

The appalling, substandard quality of residential aged care in Australia hit the limelight in recent years after staff spoke out and sparked a much needed

Nearly half of older adults don’t get enough protein – and that’s a problem. While a nutritionally well-rounded diet is vital at any age, and

Frailty is a serious problem for older adults and affects around half of people over 80. With its associated issues including weakness, muscle wasting, falls
Sign up for our newsletter